Personal experiences of anxiety and depression in pregnancy

What the research had to say
COPE research undertaken with 1,899 consumers, revealed that 43 per cent of individuals identified pregnancy as a challenging stage, as mental health conditions commonly arose – yet were often not expected. The most common conditions were those of anxiety and depression.
Source: Centre of Perinatal Excellence (2022) 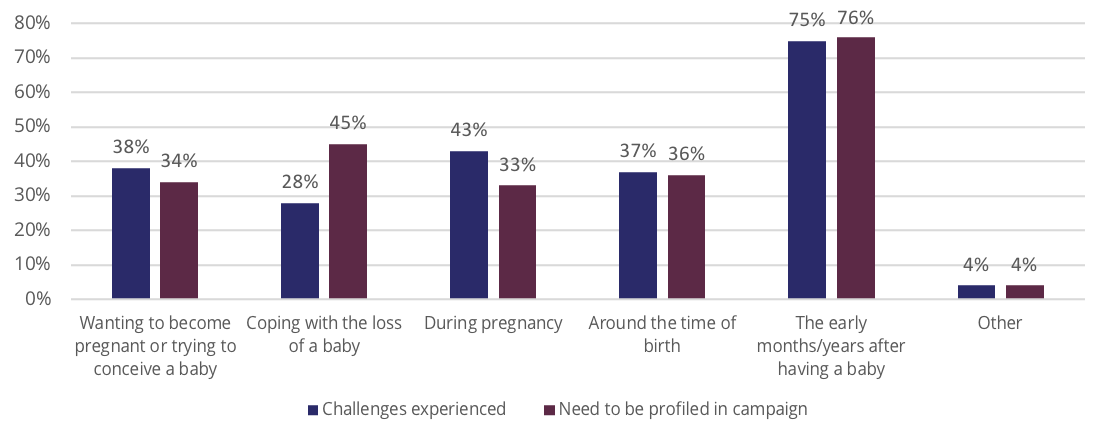
Below are the key themes identified pertaining to personal experiences of postnatal anxiety and depression. These themes informed the development of The Truth campaign.
Common symptoms of anxiety
Anxiety was experienced by many respondents. Here they described the physical symptoms as well as mental symptoms including constant worry, intrusive thoughts and rumination.
“I was anxious about everything to do with my new baby I had heart palpitations insomnia and was a pure mess”
“…My heart races, my hands tingle, I experience nausea and I also experience feelings of rage and frustration.”
“I recall feeling anxious all the time because I would worry if I was doing the right thing, if I made the right decision, if the baby would sleep, if life was always going to be this way etc.”
In some instances, this resulted in behaviours such as not being able to sleep, not leaving the house, constantly checking on their baby, and its impacts on their wellbeing in early parenthood.
“My anxiety had caused the most issues. It has prevented me from going out of the house, telling myself that my son will get hurt or something will happen. It stops me from sleeping at night, I tell myself someone’s going to break into the house and hurt my son, and I am constantly anxious about the future.”
“I felt like I was going crazy.”
In turn the physical and psychological symptoms of anxiety greatly impacted upon their functioning as a new parent and their ability to enjoy their early parenthood experience overall.
“I didn’t attach to my baby. The anxiety was crippling. I just hated it. I just had dread and a horrible sense of foreboding.
“I believe it has held me back a lot as a new parent, making it hard to believe in myself and my abilities and stops me from living in the moment and enjoying time with my child.”
Symptoms of depression – often missed
While anxiety featured more prominently than depression in pregnancy, similarly, respondents described depression experienced during pregnancy as debilitating.
“It took me to breaking point and I was prescribed anti-depressants.”
It is possible that the lower volume of responses pertaining to antenatal depression could be attributed to the fact that it was not recognised or diagnosed in pregnancy, rather, it was only detected in the postnatal period.
I didn’t know [antenatal anxiety and depression] existed so I never mentioned how I felt. I had only ever heard of PND. I felt ashamed to be feeling this way when I was fortunate enough to have conceived easily and naturally.”
Those who had experienced postnatal depression in the past, were likely to be more aware, but understandably more distressed at the thought of relapsing.
Having previously had postnatal depression, I often felt anxious about whether I’d go through that again, and if so, whether I was strong enough to survive it.”
The perception that taking medication for depression and/or anxiety during pregnancy should be avoided, is also likely to have prevented early help-seeking, access to, or continuation of medical intervention (medication).
Coming off my SSRIs abruptly when I learned I was pregnant and not being able to turn to smoking or drinking as a crutch (made my experience worse).”
A more informed GP who understood that Sertraline is a safer option for women in pregnancy with pre-existing MH issues is better than complete withdrawal during pregnancy!”
This highlights the need to reassure patients and educate health professionals that some classes of medication are safe and effective to use in pregnancy.